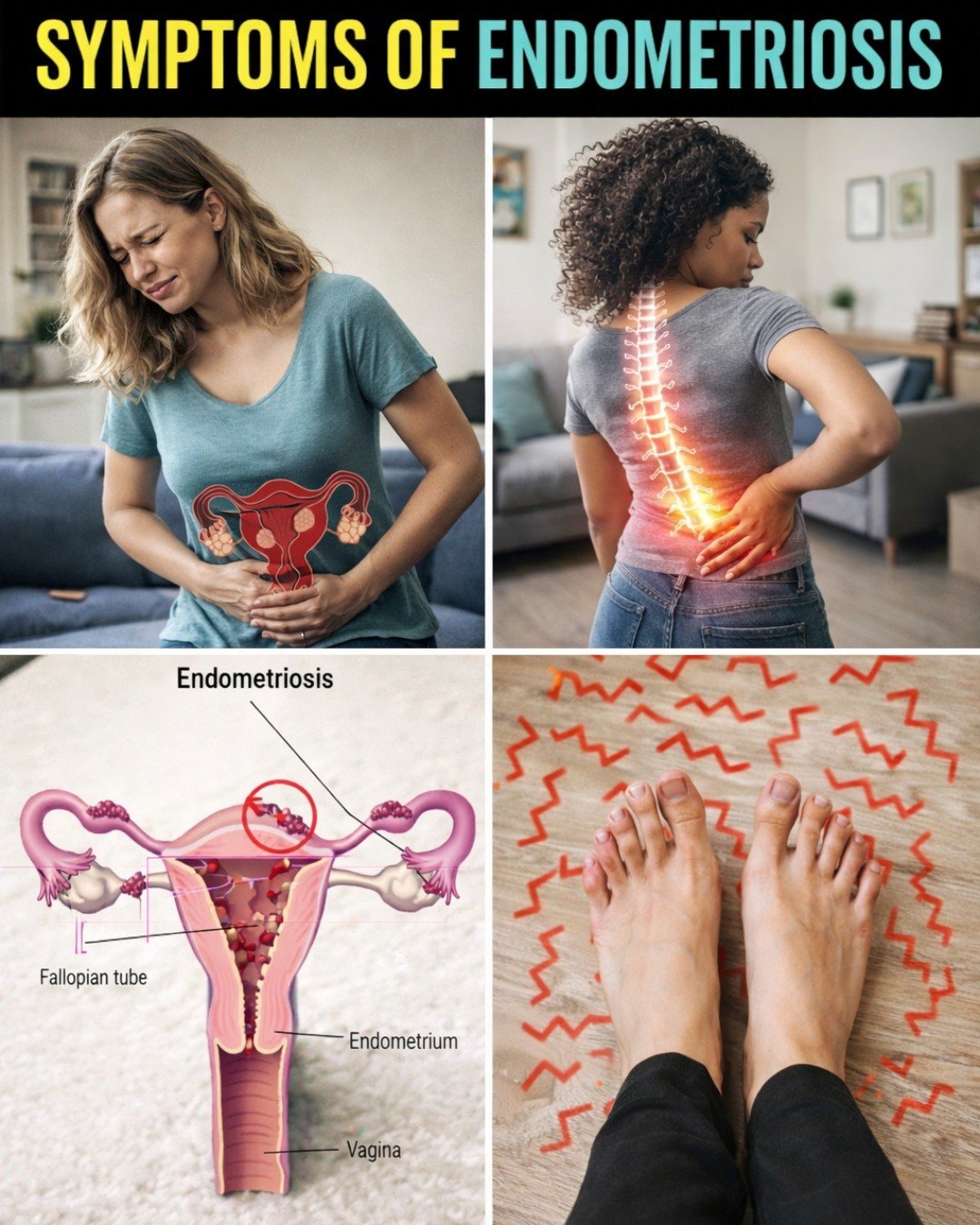
13 Warning Symptoms of Endometriosis You Ignore Daily: Is Your Pain Normal?
The silent struggle of debilitating period pain and chronic exhaustion is a reality for millions of women who are told to “just push through it.” Dismissing severe cramps as a typical part of womanhood often masks a complex condition where tissue similar to the uterine lining grows where it doesn’t belong, leading to internal scarring and silent inflammation. This normalization of suffering is precisely why many endure a diagnostic delay of 7 to 10 years, allowing the condition to progress while they search for answers. Fortunately, recognizing the subtle whispers of your body before they become screams is the first step toward reclaiming your quality of life. But as we dive into these symptoms, pay close attention to the final warning sign—it is the one most often dismissed by doctors, yet it holds the key to long-term health.

Why Endometriosis Symptoms Are Frequently Overlooked
Endometriosis affects approximately 10% of women of reproductive age, yet it remains one of the most misunderstood conditions in modern medicine. Because the symptoms often mimic other issues like Irritable Bowel Syndrome (IBS), Pelvic Inflammatory Disease (PID), or even standard PMS, patients are frequently misdiagnosed.
Studies show that inflammation caused by endometriosis isn’t just “local”; it can affect the entire body’s immune response. This is why you feel “systemically” unwell, rather than just having a “bad period.”
The Hidden Connection
Many women assume their symptoms are isolated incidents. However, endometriosis is a progressive condition. What starts as a painful cycle in your teens can evolve into chronic, daily pain by your 30s.
13 Warning Signs You Should Never Ignore
1. Debilitating Menstrual Cramps (Dysmenorrhea)
This isn’t your average “chocolate and heating pad” cramp. We are talking about pain that leaves you bedridden and unresponsive to over-the-counter painkillers.
According to the Mayo Clinic, this is the hallmark symptom. The pain often starts several days before your period and can linger long after the bleeding stops. If you are missing work or school every month, your body is trying to tell you something.

2. Chronic Pelvic Pain Throughout the Month
Does your pelvis feel heavy or “achy” even when you aren’t on your period? This is a major red flag.
The Cleveland Clinic highlights that as endometriosis progresses, lesions can cause constant irritation in the pelvic cavity. This leads to a persistent dull roar of pain that never truly goes away, regardless of where you are in your cycle.
3. Pain During or After Intercourse (Dyspareunia)
This is a sensitive topic, but a vital one. Pain during intimacy is not “normal.”
The pain is often described as a deep, stabbing sensation rather than superficial discomfort. This happens because the movement can pull on or irritate endometrial adhesions behind the uterus or on the ligaments.
Important Note: If you find yourself avoiding intimacy due to fear of pain, it is time to consult a specialist.
4. Heavy or Prolonged Menstrual Bleeding
If you find yourself changing a high-absorbency pad or tampon every hour, or passing large clots, you are experiencing menorrhagia.
Endometriosis often correlates with heavy flows and spotting between periods. This excessive blood loss doesn’t just cause discomfort—it leads to the next symptom on our list.
5. Extreme Fatigue and Brain Fog
Have you ever felt “tired in your bones” even after 8 hours of sleep? Chronic inflammation requires a massive amount of energy from your immune system.
Research suggests that the body’s constant effort to fight the lesions leads to systemic exhaustion. This isn’t just “feeling sleepy”; it’s a profound fatigue that clouds your thinking and drains your motivation.
6. Painful Bowel Movements (The “Lightning” Pain)
Many women describe a “lightning bolt” sensation in the rectum during their period.
Because the endometrial tissue can grow on the bowel or the rectovaginal septum, digestion becomes a nightmare during your cycle. You might experience:
- Painful straining.
- Diarrhea or constipation that only happens during your period.
- Cyclical bloating (often called “Endo Belly”).

7. Urinary Issues and Bladder Pressure
Is there a constant urge to pee, or does it burn when you go, even if you don’t have a UTI?
If the tissue grows near the bladder or ureters, it can cause significant irritation. This symptom is frequently misdiagnosed as Interstitial Cystitis, so tracking the timing with your cycle is crucial.
8. Lower Back, Hip, and Leg Pain
Endometriosis doesn’t stay in a neat little box in your abdomen. It often radiates.
Inflammation can irritate the sciatic nerve or other nerves in the pelvic floor. This results in a deep ache in the lower back or pain that shoots down the thighs, making it difficult to walk or stand for long periods.
9. Difficulty Getting Pregnant (Infertility)
For some women, the first sign of endometriosis is the inability to conceive.
It is estimated that 30% to 50% of women with endometriosis struggle with infertility. The condition can cause physical blockages in the fallopian tubes or create an inflammatory environment that affects egg quality.
10. Nausea and Digestive Upset
But that’s not all. The hormonal shifts and proximity of lesions to the gut often cause intense nausea.
Many patients report feeling “seasick” or losing their appetite entirely during their period. This is often dismissed as a stomach flu or “bad hormones,” but if it happens every month, it’s a pattern.
11. Irregular Spotting
If you see blood at random times of the month, your hormones are likely out of balance.
Endometriosis creates a hormonal “feedback loop” that can disrupt your natural cycle, leading to unpredictable spotting that makes it impossible to plan your life.
12. Mood Changes and Anxiety
Living with chronic pain is an emotional burden. However, the inflammation itself can affect your neurotransmitters.
It is common to feel a sense of isolation or depression when your pain is invisible to others. This emotional toll is a legitimate symptom of the disease’s impact on your central nervous system.

13. Symptoms That Worsen Over Time
This is the most critical sign. Endometriosis is generally a progressive disease.
If your “bad periods” at age 18 have turned into “bad weeks” at age 25 and “bad months” at age 30, you are seeing the progression of the disease.
Comparison Table: Normal vs. Endometriosis
| Feature | Normal Period | Endometriosis Signs |
| Pain Level | Manageable with Ibuprofen | Debilitating; interferes with life |
| Duration | 3–7 days | Pain begins before & lasts after |
| Bleeding | 2–3 tablespoons total | Heavy flow/Large clots |
| Bowel/Bladder | Occasional mild bloating | Sharp pain, diarrhea, or urgency |
| Energy | Mild tiredness | Chronic, crushing exhaustion |
Export to Sheets
Actionable Steps: What You Can Do Right Now
If these signs resonate with you, don’t panic. Knowledge is your best tool for advocacy. Follow these steps:
- Start a Symptom Journal: Track your pain, flow, and digestive issues for at least three cycles. Use an app or a notebook.
- Use Specific Language: When talking to a doctor, don’t just say “it hurts.” Use words like “stabbing,” “throbbing,” or “radiating.” Tell them exactly what activities you cannot do.
- Seek a Specialist: Many general OBGYNs are not trained in the advanced excision surgery required for endometriosis. Look for a “Migrating Endometriosis Specialist.”
- Anti-Inflammatory Diet: While not a cure, many women find relief by reducing gluten, dairy, and processed sugars which can flare inflammation.
Frequently Asked Questions (FAQ)
Can endometriosis be cured? There is currently no permanent cure for endometriosis, but it can be managed effectively through laparoscopic excision surgery, hormonal therapies, and lifestyle changes. Early intervention is key to preventing further scarring.
Does endometriosis always cause infertility? No. Many women with endometriosis go on to have healthy pregnancies. However, because it can affect the pelvic environment, it is wise to discuss fertility goals with your doctor early on.
Can an ultrasound see endometriosis? Not always. Standard ultrasounds often miss “superficial” endometriosis. While advanced MRIs or specialized ultrasounds can sometimes detect deep infiltrating lesions, the “gold standard” for diagnosis remains laparoscopic surgery.
The Path Forward
The truth is, your pain is real, and it deserves a name. By identifying these 13 warning signs, you are already ahead of the average diagnostic curve. You don’t have to accept a life of “powering through” agony.
In our next guide, we will reveal the “Golden Window” for treatment—the specific timeframe where intervention can most effectively protect your fertility and stop the progression of the disease. You won’t want to miss how a simple change in your daily routine can significantly dampen the “Endo flare” before it even starts.
Disclaimer: This article is for informational purposes only and does not constitute medical advice. Always seek the advice of your physician or other qualified health provider with any questions you may have regarding a medical condition.
Would you like me to create a personalized symptom-tracking template or find specialized treatment centers in your area?