Breast cancer continues to affect millions of women around the world each year, and unfortunately, many cases are still found at more advanced stages when treatment options can become more complex. In the rush of daily life—balancing work, family, and everything in between—it’s all too easy to overlook subtle shifts in your body that could be important signals. The fear of “what if” can feel heavy, but here’s the reassuring truth: most breast changes turn out to be harmless, and noticing potential early clues gives you real power to act quickly. Research from trusted organizations like the American Cancer Society and Mayo Clinic shows that paying attention to these quieter signs can make a real difference in outcomes.
But that’s not all… at the end of this article, I’ll share one simple daily habit that many women skip—but that can help you spot differences much sooner (and it’s easier than you think).

Why Early Awareness Matters More Than You Think
Most early breast cancers don’t cause pain right away. That’s why it’s common for women to feel “everything’s fine” when there’s no discomfort. Studies show that subtle signals can appear months—or sometimes longer—before a lump becomes noticeable. Recognizing these changes early allows you and your doctor to investigate promptly, often when options are simplest and most effective.
The good news? Many of the most meaningful clues aren’t even about finding a lump.
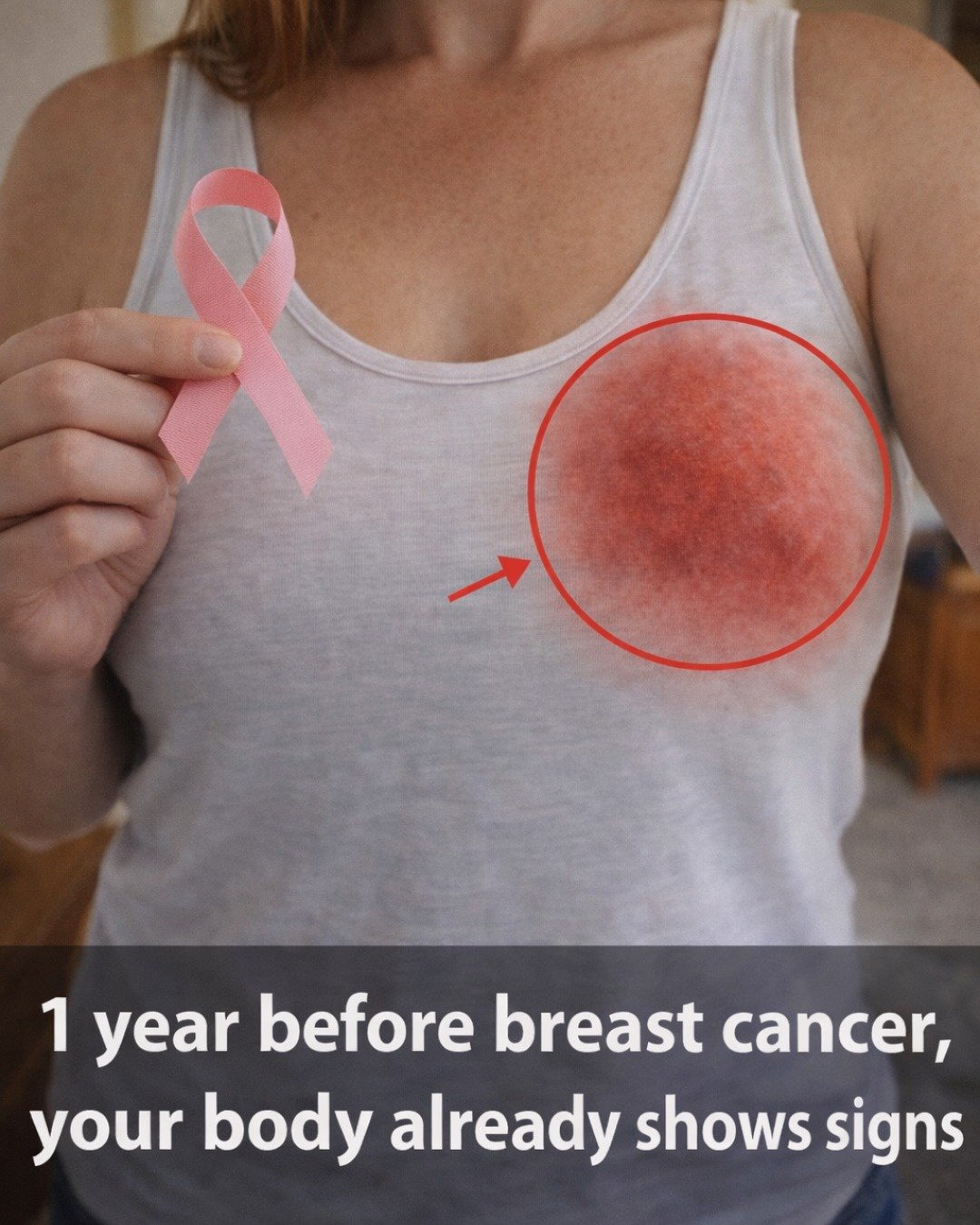
1. Changes in Breast Skin Texture or Appearance
Your breast skin can sometimes reveal the earliest hints that something needs attention.
Common skin-related signs include:
- Dimpling or puckering — skin that resembles the texture of an orange peel (known medically as peau d’orange)
- Unexplained redness, rash, or flaky skin on part of the breast that persists
- Thickening or a sudden change in texture on one breast (compared to the other)
- New, ongoing itching in a specific spot
Many women first spot these while dressing, showering, or applying lotion. These changes can stem from benign issues like irritation or infection—but if they last more than 2–3 weeks and affect only one breast, it’s worth getting checked. Organizations like the CDC and American Cancer Society list skin irritation or dimpling as key warning signs to take seriously.
2. Nipple Changes You Shouldn’t Ignore
The nipple and the surrounding darker area (areola) can provide very early clues.
Watch for these important changes:
- A nipple that suddenly pulls inward (inversion) when it used to point outward
- Scaling, flaking, crusting, or redness on the nipple or areola
- New discharge from the nipple — especially if it’s bloody, clear, or happens without squeezing (and from only one breast)
- The nipple pointing in a new or different direction
Important note: Discharge from both breasts that only occurs when squeezed is often normal (particularly in women who’ve been pregnant). However, spontaneous, one-sided discharge is more concerning and should prompt a visit to your doctor.

3. Changes in Size, Shape, or Symmetry
Breasts are rarely perfectly symmetrical, but a recent, noticeable difference between the two can be significant.
Pay attention if you notice:
- One breast suddenly becomes larger or smaller (without recent weight changes)
- Visible swelling in one breast, even when you’re not near your period
- A shift in the overall shape or contour of one breast
- One side feeling heavier or more “full” than usual
Here’s a practical tip many women find helpful: take a quick photo of your breasts in the mirror once a month (same lighting and angle). This simple habit helps reveal subtle changes that daily glances might miss.

4. Persistent Pain or Discomfort in One Specific Spot
While early breast cancer is often painless, some women do experience discomfort worth noting.
Look out for:
- A constant dull ache or sharp pain in one specific area that doesn’t follow your menstrual cycle
- Tenderness that stays in the same spot for weeks
- Discomfort that feels unlike your usual hormonal breast sensitivity
Key difference: Cycle-related tenderness usually affects both breasts and comes and goes. Pain that’s localized, persistent, and unrelated to hormones deserves evaluation, as noted in guidelines from major health organizations.

The Simple Daily Habit That Helps You Notice Changes Earlier
Here’s the overlooked practice experts now emphasize: monthly breast self-awareness (not the rigid old self-exam routine that major groups like the American Cancer Society no longer recommend as mandatory).
The goal is simple—become familiar with what “normal” feels and looks like for your breasts, so you quickly spot anything different.
Try this easy 5-minute routine:
- Choose a consistent day each month (e.g., the first day after your period ends, or the same calendar date if postmenopausal).
- Stand in front of a mirror: Check visually with arms at your sides, then arms raised, and again while leaning forward.
- Use the flat pads of your fingers (not tips) to feel each breast in a pattern—up-and-down lines, circles, or wedges—covering the whole area.
- Gently squeeze the nipple to check for any discharge.
- Feel above the collarbone and in the armpit area for any changes.
This isn’t about hunting for cancer—it’s about knowing your body better. Any new or unusual change? Report it to your healthcare provider right away.
When Should You See a Doctor?
Don’t wait if you notice:
- Any skin, nipple, size/shape, or persistent pain changes lasting more than 2–3 weeks
- A new lump, thickening, or area that feels different
- Spontaneous nipple discharge (especially bloody or one-sided)
Most changes are benign—especially in younger women—but checking them out brings peace of mind and, when needed, earlier support.
Frequently Asked Questions (FAQ)
Can men get breast cancer too?
Yes, though it’s much rarer. Men can notice the same signs (like lumps, skin changes, or nipple discharge) and should see a doctor if anything feels off.
I’m under 40—do I still need to pay attention?
Absolutely. While risk rises with age, breast cancer can happen younger. Building awareness of your normal breasts is valuable at any age.
How often should I get a mammogram?
Guidelines vary by country and personal risk. Many organizations recommend discussing screening with your doctor, often starting around age 40–50. Your provider can help tailor what’s best for you.
Final Thoughts
Your body often whispers warnings long before anything becomes obvious. By staying tuned to these four early signs—skin changes, nipple differences, size/shape shifts, and persistent localized discomfort—you give yourself the best chance to act early if something seems different.



2 thoughts on “4 Early Warning Signs of Breast Cancer Women Should Never Ignore”