Did you know you can do “everything right” and still feel unsure about your breath? You brush, you floss, you pop a mint before a close conversation—and then, out of nowhere, that strange foul taste shows up again. If you’ve ever rated your breath confidence below an 8 out of 10, keep reading, because the reason might be hiding in plain sight.
Picture a normal evening. You’re eating, laughing, mid-sentence—and a tiny, hard white chunk dislodges in your mouth. The taste is unmistakable: sour, sulfur-like, and instantly alarming. It’s not your imagination. It’s a sign many adults experience but rarely talk about. And the most surprising part is how common it may be.
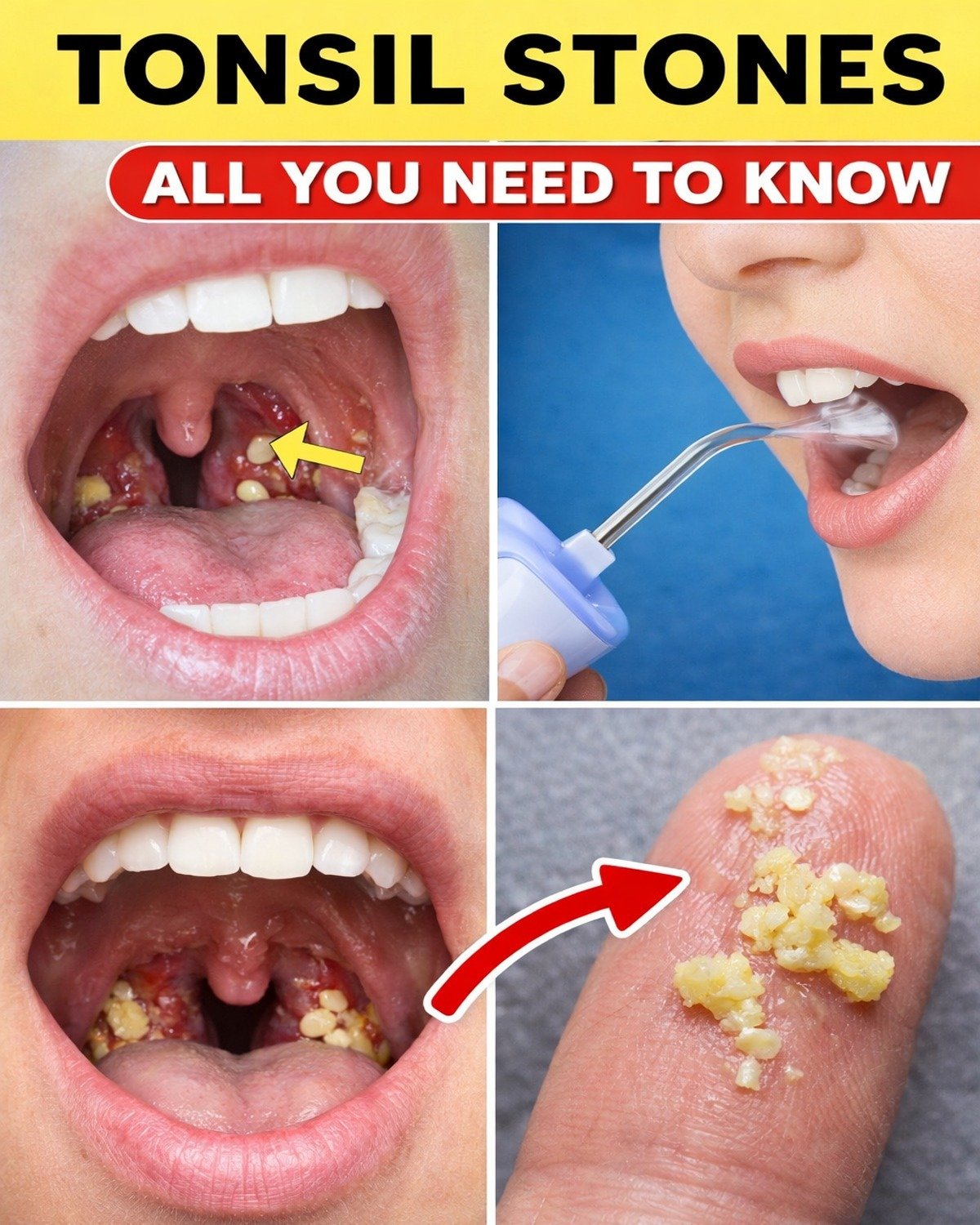
Tonsil stones—also called tonsilloliths—can quietly build in the crevices of your tonsils. They can trigger bad breath, throat irritation, and that “something stuck” feeling that makes swallowing feel weird. But what if you could manage them with practical, science-informed habits that fit real life? Stay with me, because the most effective strategy usually isn’t the one people try first.
Why Tonsil Stones Feel So Personal (and So Frustrating)
Bad breath isn’t just a hygiene issue. It’s a confidence issue. It’s the hesitation before leaning in to talk. It’s the split-second worry during a meeting. It’s the way you may start turning your head slightly when you speak, hoping distance does the job. If that feels familiar, you’re not alone—and that matters.
Tonsil stones form when food particles, dead cells, mucus, and bacteria collect in tonsil crypts—small pockets that can deepen with age. Over time, the material can harden and develop an odor due to sulfur compounds produced by certain bacteria. You can have excellent dental care and still deal with this, because the source isn’t your teeth. It’s the trapped debris in the back of your throat.
Here’s a quick self-check before you continue: on a scale of 1–10, how confident do you feel about your breath during close conversations right now? Hold that number. The goal isn’t perfection. The goal is progress, and it can begin faster than you think.
What Tonsil Stones Are, in Plain English
Imagine your tonsils like a sponge with tiny holes. Those holes can collect bits of “stuff” from daily life—tiny food particles, thick mucus from allergies, postnasal drip, and shed cells. Add bacteria, and the mix can become a compact, chalky lump. That’s a tonsil stone.
Some people notice them as a persistent bad taste. Others feel a scratchy throat or a “lump sensation” that comes and goes. Some spot white or yellow specks near the tonsils. And plenty of people have no symptoms until a stone dislodges—often at the worst possible moment, like a date or a presentation.
If you’ve tried mints, strong mouthwash, or intense brushing and still feel stuck, it’s because those methods mostly target the front of the mouth. Tonsil stones live in the back, and they often require a different kind of approach. And yes—there are safe, gradual options to try before thinking about procedures.
The 15 Strategies That Can Change Your Routine (Without Changing Your Life)
The key is not to do all 15 at once. The real secret is stacking a few high-impact habits consistently. Start with the most realistic ones for you, because consistency beats intensity every time. And the next strategy may surprise you more than any mouthwash ever could.
1) Salt Water Gargles for Daily Reset
Laura, a 42-year-old teacher, felt self-conscious during parent meetings. She wasn’t neglecting hygiene—she was exhausted and confused. She began gargling warm salt water once daily after brushing. Within weeks, she felt more confident and noticed fewer “mystery” bad-breath moments.
Salt water may help by loosening debris through osmotic effects and temporarily shifting the oral environment in a less bacteria-friendly direction. Keep it simple: warm water, a pinch of salt, 20–30 seconds. The best part is what happens when you pair this with the next step.
2) Hydration That Keeps Mucus Moving
Dry mouth isn’t just uncomfortable—it can make debris stickier. Emma, a 50-year-old nurse on long shifts, noticed her symptoms flared when she was dehydrated. She increased water intake and set a reminder for small sips across the day. Over time, she reported fewer recurring stones.
Hydration supports saliva flow, and saliva is one of your body’s natural cleaning systems. If you’re not sure where you stand, rate your daily hydration from 1–10. If it’s under 7, you might be leaving an easy win on the table.
3) Targeted Tongue Cleaning (Not Just Brushing Teeth)
John, a 45-year-old sales rep, brushed hard and often. But he rarely cleaned the back of his tongue. Once he started gentle tongue brushing or using a tongue scraper, he noticed a fresher baseline. Why? The tongue can harbor bacteria linked to odor and biofilm buildup.
Think of it this way: if you mop only half a floor, the whole room still smells. This one change can amplify everything else you do next.
4) Warm Water in the Morning to “Wake Up” Flow
This sounds almost too simple, but a warm-water rinse or sip in the morning can reduce that sticky, dry sensation in the throat. It may help loosen overnight mucus and make your first oral-care steps more effective. It’s not a cure—just a useful nudge in the right direction.
And that’s the theme here: small nudges, stacked strategically, can shift the outcome.
5) Gentle Cough Technique to Dislodge Small Stones
Mike, a 38-year-old dad, felt that annoying “lump” sensation during dinner. Instead of aggressive poking, he tried gentle, controlled coughing after a warm drink. Some smaller stones dislodged naturally over time, and discomfort eased.
This matters because forceful digging can irritate tissue. If you try coughing, keep it gentle. If pain increases, stop. The next strategy is where prevention gets smarter.
6) Address Postnasal Drip and Nasal Congestion
For many people, the real “fuel” for tonsil stones is mucus. Allergies, chronic congestion, and postnasal drip can feed debris into tonsil crypts. Simple steps—like saline nasal rinses, managing indoor allergens, or discussing allergy control with a clinician—can reduce the source material.
If you’ve ever felt mucus sliding down your throat, you’ve felt the supply chain. Cutting it can be a turning point.
7) Choose Alcohol-Free Mouthwash When You Use One
Alcohol can dry the mouth for some people, which may backfire if dryness is a trigger. If you use mouthwash, consider alcohol-free options and avoid overdoing it. The goal is support, not scorched earth. Your mouth needs balance, not sterility.
And if you think balance sounds vague, the next tip makes it concrete.
8) Probiotic Foods to Support Oral Microbiome Balance
Tom, a 48-year-old mechanic, noticed odor spikes even with cleaning. He added plain yogurt and other probiotic foods consistently. Over a month, he felt more stable breath comfort. Research is still evolving, but the idea is that beneficial bacteria may help compete with odor-producing strains.
It’s not about one miracle food. It’s about shaping an ecosystem, and ecosystems respond to patterns.
9) Low-Pressure Water Flosser, Used Carefully (If You’re Comfortable)
Lisa, a 39-year-old executive, used a water flosser cautiously at the lowest setting, focusing on oral cleaning rather than blasting the tonsils. Some people use gentle irrigation to reduce debris in the mouth overall, which can indirectly reduce what reaches the tonsils.
Important note: direct tonsil irrigation can be risky if done aggressively. If you’re unsure, skip this and choose other steps first. Your throat deserves respect.
10) Dietary Tweaks That Reduce Mucus Triggers (When Relevant)
Some people notice more mucus or thicker saliva after certain foods, especially if sensitive to dairy or high-sugar snacks. Ben, a 52-year-old chef, experimented with reducing sugary snacks and monitoring dairy. His recurrence seemed to drop.
This isn’t a universal rule. It’s a “notice your pattern” rule. Try a 2-week experiment, not a lifetime restriction, and see what your body says.
11) Practice “After-Meal Rinsing” to Reduce Residue
A quick water rinse after meals can reduce lingering particles that may later contribute to tonsil debris. It’s simple, fast, and surprisingly effective when done consistently—especially after sticky foods.
You don’t need perfection. You need a repeatable routine.
12) Manage Acid Reflux If It’s Part of Your Story
Silent reflux can irritate the throat and may contribute to mucus changes or tonsil discomfort. If you often have throat clearing, a sour taste, or symptoms that worsen at night, it may be worth discussing reflux strategies with a clinician. Small changes like not eating right before bed can help some people.
If that resonates, keep going—because now we enter the “when to get expert help” zone.
13) Get an ENT Evaluation When Symptoms Persist
If you have frequent stones, significant pain, one-sided swelling, recurrent infections, bleeding, or trouble swallowing, it’s time for a professional evaluation. An ENT can confirm what’s happening and rule out other causes of bad breath or throat symptoms.
Peace of mind is a health strategy too, and it can prevent unnecessary self-treatment.
14) Laser Cryptolysis as a Minimally Invasive Option
For people with recurrent stones, some ENTs offer laser cryptolysis, which may reduce the depth of tonsil crypts so debris has fewer places to lodge. Recovery can be shorter than more invasive options, though it’s not right for everyone.
If you’re thinking, “I want a long-term fix,” you’re not alone. There’s one more step.
15) Coblation or Tonsillectomy in Select Cases
Coblation is another technique that may reduce crypt depth with less heat damage than traditional approaches. In severe or recurrent cases, tonsillectomy is a definitive option—but it involves a more intense recovery and must be considered carefully with medical guidance.
The real takeaway isn’t that everyone needs a procedure. It’s that you have a spectrum of options, and you can choose based on severity, recurrence, and professional input.
Two Quick Tables to Make This Actionable
| Common Problem | Typical Quick Fix | Why It Often Fails | More Helpful Direction |
|---|---|---|---|
| Bad breath spikes | Mints/gum | Masks odor, doesn’t remove debris | Gargles + tongue cleaning |
| Throat “lump” feeling | Lozenges | Soothes temporarily | Hydration + mucus management |
| Recurrence | Random remedies | Inconsistent approach | Habit stacking |
| Dry mouth | Strong mouthwash | Can worsen dryness | Alcohol-free + hydration |
| Anxiety about breath | Avoidance | Builds stress | Track triggers + routine |
| Timeline | What to Try | What You Might Notice |
|---|---|---|
| Days 1–7 | Salt gargle + hydration | Less bad taste, less dryness |
| Week 2 | Tongue cleaning + rinsing after meals | More stable breath confidence |
| Weeks 3–4 | Address mucus triggers + probiotic foods | Fewer recurrences for some |
| Ongoing | Consistent routine + ENT if needed | Long-term control and clarity |
If you’ve made it this far, pause for a 10-second check-in. Rate your throat comfort right now on a scale of 1–10 compared to when you started reading. Even if nothing changed yet, your awareness just did. And awareness is the beginning of control.
Your Clear Path Forward: Start With One Move Tonight
Here’s the plot twist most people miss: the “best” strategy isn’t the most intense one. It’s the one you’ll actually repeat. Tonsil stones thrive on neglect and inconsistency. They shrink when your routine becomes steady.
Start tonight with one action you can commit to for 7 days. Maybe it’s warm salt water gargling. Maybe it’s a hydration target. Maybe it’s tongue cleaning. Pick one, and make it automatic. Then stack a second habit next week.
Imagine 30 days from now: you’re closer in conversations, less hesitant, less distracted by that nagging throat sensation. That change can feel bigger than you expect, because it’s not only physical. It’s social confidence returning.
And if you’re dealing with frequent recurrence, significant pain, or swelling—don’t white-knuckle it alone. A professional evaluation can bring clarity fast, and sometimes clarity is the most comforting remedy of all.
P.S. Warm lemon water in the morning can feel soothing for some people and may support hydration, but if you’re prone to reflux or enamel sensitivity, consider plain warm water instead. The best routine is the one your body agrees with.
This article is for informational purposes only and does not replace professional medical advice. Consult your healthcare provider for personalized guidance.