Many women brush off irregular spotting, unusual discharge, or nagging aches as just part of a busy life or hormonal shifts, but these subtle changes can sometimes point to deeper health concerns that deserve attention. The constant worry about what’s normal and what isn’t can leave you feeling anxious and exhausted, especially when daily routines get disrupted by unexplained discomfort. The good news is that simple awareness paired with routine check-ups can help you stay ahead of potential issues.
But here’s the part most women miss until later: one overlooked clue often appears in everyday moments and can be your strongest nudge to act fast – keep reading because we’ll share exactly how to respond and protect yourself long before anything escalates.
Why Early Awareness Matters for Every Woman
Cervical cancer often starts quietly, with no obvious clues in its earliest stages. That’s exactly why health experts from the Mayo Clinic and Centers for Disease Control and Prevention stress regular screenings over waiting for symptoms to appear.
When changes do show up, they can feel easy to dismiss as stress, menopause, or minor infections. Yet paying attention early gives you the best chance to discuss concerns with your doctor. This isn’t about fear – it’s about feeling empowered and informed.
The 9 Warning Signs Most Women Overlook
Here are the most common signs drawn from trusted medical sources. Remember, these can have many causes, so they’re simply signals to check with a healthcare professional.
1. Bleeding after intercourse
Even light spotting after sex can feel surprising. Many women chalk it up to dryness or rough activity, but it’s one of the top clues experts flag first.
2. Bleeding between periods
Random bleeding outside your usual cycle often gets blamed on birth control or stress. Yet it’s a red flag worth noting because it disrupts what your body considers normal.
3. Bleeding after menopause
Any bleeding once periods have stopped for a full year should never be ignored. This one surprises many women who assume everything is finally “settled.”
4. Heavier or longer periods than usual
If your flow suddenly feels heavier or lasts days longer, it’s easy to blame age or diet. But tracking changes helps you spot patterns early.
5. Unusual vaginal discharge
Watery, pink, brown, or foul-smelling discharge that appears between cycles or after menopause often gets mistaken for normal variation. The American Cancer Society notes this as a frequent early clue.
6. Pain during intercourse
Discomfort or sharp pain that wasn’t there before can feel embarrassing to mention. Yet it’s a common signal that deserves an open conversation with your doctor.
7. Persistent pelvic or abdominal pain
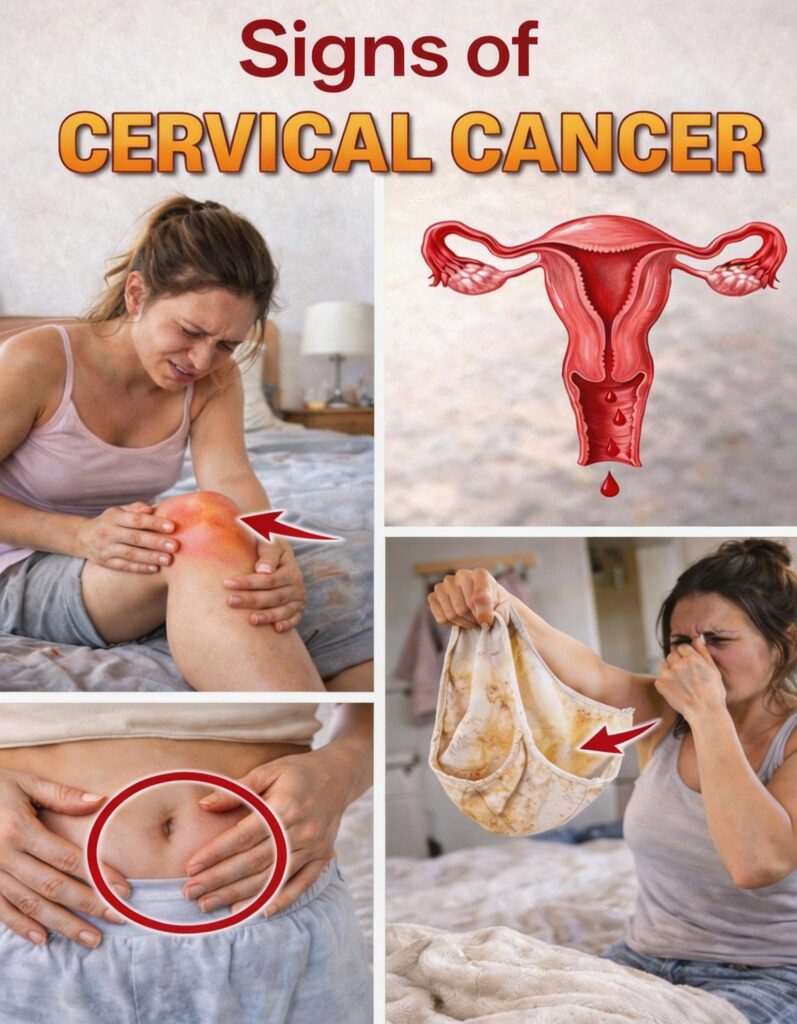
A dull ache in your lower belly that lingers for weeks can be blamed on digestion or exercise. The image many women recognize shows hands clutching the abdomen exactly like this.
8. Lower back or leg pain
Unexplained pain radiating to the back or even knees and legs (as shown in health illustrations with a red arrow on the knee) sometimes appears when issues progress. Swelling in one leg can accompany it.
9. Difficulty urinating or having bowel movements
Feeling like you can’t fully empty your bladder or sudden changes in bowel habits can seem unrelated. In more advanced cases, these join the list of signals to discuss promptly.
But wait – that’s not the whole story. The real power comes from what you do next.
Actionable Steps You Can Take Right Now
Here’s a simple 5-step plan any woman can start today. These habits support overall cervical health without promising miracles.
- Schedule your next screening – Pap tests or HPV tests are quick and recommended every 3–5 years for most women aged 21–65.
- Track your symptoms – Use a phone note or app to log any unusual bleeding, discharge, or pain for two weeks before your appointment.
- Discuss family history – Share any history of HPV or cervical issues with your doctor so they can tailor advice.
- Consider the HPV vaccine if eligible – It’s still helpful for many adults under 45 and protects against the main cause.
- Adopt supportive habits – Eat plenty of fruits and vegetables, stay active, and avoid smoking to keep your immune system strong.
These small actions add up and give you peace of mind.
How Screening Changes Everything
The most surprising part? Many cases are found and handled long before any of these signs appear. Regular pelvic exams combined with modern testing catch changes years ahead of time. That’s why experts call cervical cancer one of the most preventable cancers when women stay consistent with check-ups.
You don’t need to live in fear. You simply need the right information and a plan.
What This Means for You Today
Paying attention to your body doesn’t mean panicking at every twinge. It means becoming your own best advocate. The women who catch things early often say the same thing: “I wish I’d known sooner, but I’m glad I finally listened.”
Start with one step this week – book that appointment or begin tracking. Your future self will thank you.
FAQ About Cervical Cancer Signs
Can these signs mean something else besides cervical cancer?
Absolutely. Infections, fibroids, endometriosis, or hormonal changes cause many of the same symptoms. Only a doctor can determine the cause through proper testing.
How often should I get screened if I feel healthy?
Most women 21–29 need a Pap test every 3 years. From age 30–65, combining Pap and HPV testing every 5 years is common. Your doctor will personalize based on your history.
Is there anything I can do to lower my risk besides screening?
Yes – the HPV vaccine, not smoking, practicing safer sex, and maintaining a healthy weight all support lower risk. Talk with your provider about what fits your life.
Disclaimer: This article is for informational and educational purposes only. It is not a substitute for professional medical advice, diagnosis, or treatment. Always consult your healthcare provider if you experience any concerning symptoms or changes in your body. Individual results and health needs vary.