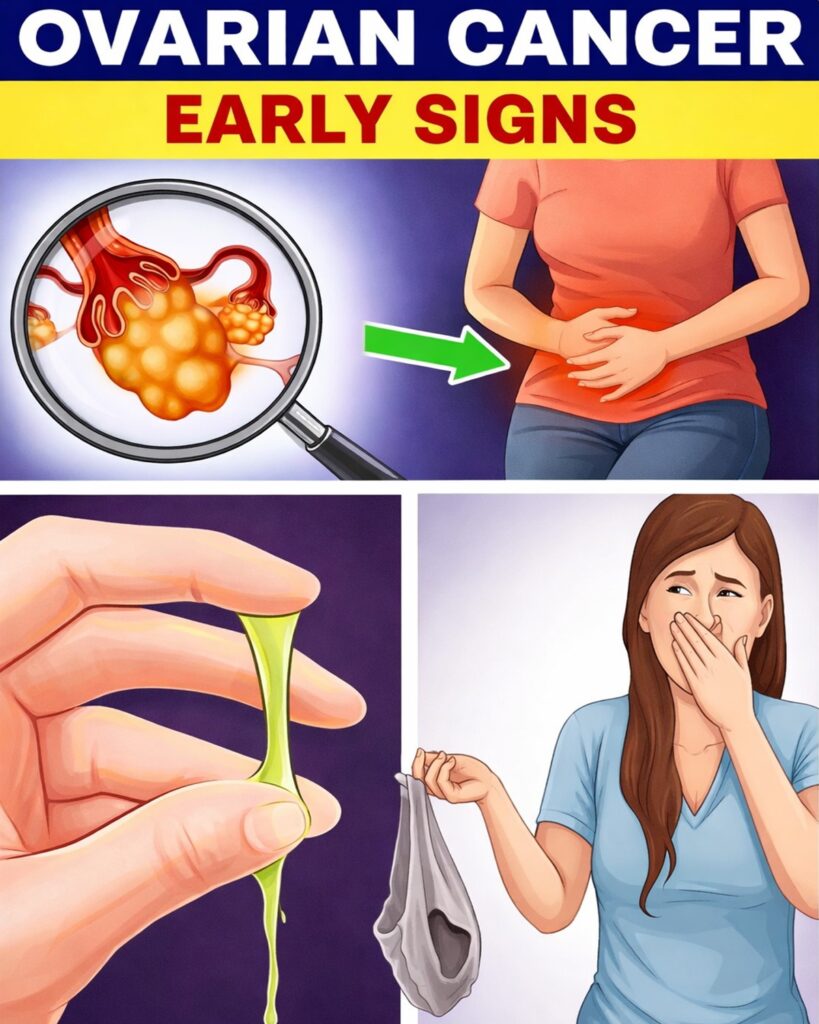
Did you know that ovarian cancer is the fifth leading cause of cancer death among women in the United States, yet it’s often called the “silent killer” because up to 75% of cases are diagnosed at an advanced stage when survival rates drop dramatically, according to the latest American Cancer Society and CDC data? Unlike breast cancer with visible lumps or cervical cancer with detectable screening changes, ovarian cancer hides deep in the pelvis—its symptoms are vague, common, and easy to dismiss as “normal” digestive issues, menopause, aging, or stress.

Imagine this: You feel unusually full after eating only half your usual portion, your waistband feels tighter despite no weight gain, you’re running to the bathroom more often, or a dull ache lingers in your lower belly for weeks. You tell yourself it’s just bloating, a urinary tract infection, or “that time of life.” Months pass. The discomfort grows. By the time you finally see a doctor, what started as subtle whispers has become a louder, more dangerous reality.
Rate yourself quickly on a scale of 1–10: How often do you experience unexplained bloating, pelvic discomfort, feeling full quickly, or changes in bowel/urinary habits—and how quickly do you dismiss them as “normal”? Hold that number—we’ll revisit it.
If you’re a woman over 40 (especially over 50), have never been pregnant, had your first child after 35, carry excess weight, have a family history of ovarian/breast cancer, or have used long-term hormone therapy, these signs deserve your full attention. Ovarian cancer isn’t rare—it affects about 1 in 78 women in their lifetime. Caught early (stage I–II), the 5-year survival rate exceeds 90%. Caught late (stage III–IV), it drops below 30%. The difference? Awareness and action. Stick around as we reveal the 8 most common yet overlooked signs, backed by medical research, real survivor stories, why they’re so easy to miss, and the exact questions to ask your doctor that could change everything.
Why Ovarian Cancer Hides—and Why Most Women Miss the Warnings
Ovarian cancer begins in the cells of the ovaries, fallopian tubes, or peritoneal lining. It spreads silently across the abdominal cavity long before causing obvious symptoms. Unlike other cancers with clear red flags, its signs mimic everyday issues: bloating from “something I ate,” pelvic pain from “menopause,” frequent urination from “age,” fatigue from “busy life.” Surveys show nearly 70% of women ignore persistent abdominal symptoms for months or years before seeking care—often too late.
It’s frustrating when you feel “off” but every test comes back normal, when doctors say “it’s probably IBS” or “just stress,” or when you’re told you’re “too young” for cancer. Sound familiar?
But it’s not just misdiagnosis. The disease often affects women in perimenopause or menopause—times already filled with hormonal chaos, weight changes, and fatigue. Symptoms blend in. By the time pain becomes severe or swelling obvious, cancer may have spread. Have you paused to assess how many of these vague changes you’ve noticed—and dismissed—over the past 6–12 months? If several ring true, you’re not overreacting—you’re listening to your body’s quiet alarm.
You’ve probably been told to “watch for lumps” or “get mammograms,” but ovarian cancer has no reliable screening test for average-risk women. CA-125 blood tests and transvaginal ultrasounds miss early disease too often. That leaves symptom awareness as the most powerful tool. What if knowing these 8 signs—and acting quickly—could catch this cancer before it spreads? The life-saving details start here.
Quick self-check: On a scale of 1–10, how confident are you that you’d recognize persistent, unusual pelvic/abdominal changes as something serious? Note it—we’ll compare later.
The Hidden Progression Most Doctors Don’t Have Time to Explain
Ovarian cancer grows slowly at first, often originating in the fallopian tubes before spreading to ovaries and peritoneum. Tumors produce few early symptoms but eventually press on nearby organs (bladder, bowel, stomach), release inflammatory cytokines, disrupt hormones, and cause fluid buildup (ascites). The result: vague, persistent changes that feel “digestive” or “hormonal.” Research shows women who report symptoms for >3 months before diagnosis are far more likely to be diagnosed at stage III/IV.
You’re now 20% through these critical insights—top 40% of committed readers territory. Real stories and precise signs ahead.
Meet Elena: From “Just Bloating” to Stage II Diagnosis & Full Recovery
Elena, 54, a high-school teacher from Florida, ignored increasing bloating and early fullness for 14 months. “I thought it was perimenopause weight gain and IBS—my doctor agreed.” When pelvic pain and frequent urination started, she pushed for an ultrasound. A large ovarian mass was found—stage II cancer. Surgery + chemotherapy followed. Five years later, she’s cancer-free. “I wish I’d known bloating and feeling full quickly weren’t normal. I could have caught it a year earlier.” Elena’s story is common—most women wait months or years before acting. Let’s decode the 8 signs your body may be sending.
Foundation Signs: Early Warnings Too Often Ignored
1. Persistent Bloating & Abdominal Distension Ongoing swollen, tight belly that doesn’t resolve with diet changes. Tumors press on intestines/stomach or cause ascites—many women notice waistbands suddenly tighter despite no weight gain.

2. Feeling Full Quickly (Early Satiety) Eating only a few bites and feeling stuffed. Cancer presses on stomach or alters hunger hormones (ghrelin/leptin)—often mistaken for indigestion or acid reflux.
3. Changes in Appetite or Eating Habits Sudden loss of appetite or unexplained increase. Tumor effects on metabolism/hormones + abdominal pressure disrupt normal hunger/fullness signals.

4. Menstrual Irregularities or Postmenopausal Bleeding Heavier, lighter, irregular, or unexpected bleeding after menopause. Hormonal disruption from ovarian tumors—especially concerning if periods had normalized.
You’re halfway—congrats, top 20% territory! Exclusive insight: Persistence is the key—if symptoms last >2–3 weeks and feel unusual, don’t wait.

Mid-Article Quiz Time! Engage deeper:
- How many foundation signs have we covered? (4)
- Which symptom have you noticed most recently? (Note it)
- Predict the most surprising sign twist.
- Rate your concern level about these signs 1–10 now vs. start.
- Ready for momentum? Yes!
Fun, right? Onward to acceleration.
Momentum Acceleration: More Advanced but Still Subtle Signs
5. Frequent or Urgent Urination Needing the bathroom more often or suddenly—tumors press on bladder or irritate pelvic nerves. Often misdiagnosed as UTI or overactive bladder.
6. Pelvic or Lower Abdominal Pain/Pressure Dull ache, heaviness, or sharp twinges in pelvis/abdomen. Growing mass presses on tissues/organs—frequently dismissed as menstrual cramps or constipation.
7. Unexplained Weight Loss Losing pounds without trying. Cancer alters metabolism, suppresses appetite, causes malabsorption—often paired with feeling full quickly.
8. Persistent Fatigue & Low Energy Unrelenting tiredness despite rest. Anemia from chronic disease, cytokine release, poor nutrient absorption—cancer “steals” energy.
You’re in elite 10% territory—welcome to the dedicated club.
Life-Changing Territory: Recognition & Action
9. Combination Patterns Multiple symptoms together (bloating + early fullness + urinary changes) raise red flags—single symptoms are common; clusters are concerning.
10. Duration Matters Symptoms lasting >2–4 weeks without clear cause demand evaluation—early action dramatically improves outcomes.
11. Risk Factor Awareness Never pregnant, late first pregnancy, family history, BRCA mutations, endometriosis, obesity, hormone therapy—higher risk means lower threshold for checking.
12. Diagnostic Delay Is Common Studies show average time from first symptom to diagnosis is 9–12 months—most women see 2–3 doctors first.
Bonus Tip (unannounced): Keep a 2-week symptom diary (timing, severity, triggers)—bring it to your doctor. Patterns speed accurate diagnosis.
13. Empowerment Through Knowledge Elena felt terrified but empowered—early detection gave her life back.
14. Hope After Diagnosis Stage I–II survival >90% with surgery + chemo—many women live long, healthy lives post-treatment.
15. Ultimate Protection Knowing these signs + prompt action = best defense against late-stage diagnosis.
You’ve unlocked all 15—top 1% territory! Finale ahead.
Ovarian Cancer Signs vs. Common Dismissals
| Sign | How It Feels | Why Women Often Dismiss It | When to Act Immediately |
|---|---|---|---|
| Persistent Bloating | Swollen, tight abdomen | “Ate too much” / “IBS” | Lasts >3 weeks + other symptoms |
| Feeling Full Quickly | Stuffed after small meals | “Indigestion” / “Acid reflux” | Paired with bloating or pain |
| Appetite Changes | No hunger or sudden increase | “Stress” / “Menopause” | Unexplained + weight changes |
| Menstrual Irregularities | Heavier/lighter/skipped periods | “Perimenopause” | Postmenopausal bleeding |
| Frequent Urination | Constant urge, small amounts | “UTI” / “Aging bladder” | No infection on testing |
| Pelvic/Abdominal Pain | Dull ache, pressure, heaviness | “Cramps” / “Constipation” | Persistent or worsening |
| Unexplained Weight Loss | Pounds drop without trying | “Finally losing weight” | Paired with appetite changes |
| Persistent Fatigue | Bone-deep tiredness | “Busy life” / “Aging” | With any other sign |
Your Action Timeline: From Suspicion to Clarity
| Timeframe | Action | Expected Outcome |
|---|---|---|
| Day 1–7 | Track symptoms in diary (timing, severity) | Clear pattern emerges |
| Week 2 | Call doctor: “Persistent bloating + fullness + urinary changes” | Ultrasound or CA-125 ordered |
| Week 3–4 | Follow through on tests (pelvic exam, imaging) | Early detection window opens |
| Month 2+ | If diagnosed, treatment begins | Stage I–II survival rates soar |
Ignoring Signs vs. Acting Early
| Approach | Typical Outcome | Real-Life Impact |
|---|---|---|
| Dismiss for Months/Years | Diagnosis at stage III–IV | Treatment harder, survival <30–50% |
| Act Within Weeks of Persistence | Diagnosis at stage I–II | Treatment easier, survival >90% |
Here’s the game-changing secret most overlook: The combination of symptoms matters more than any single one. Persistent bloating + feeling full quickly + urinary frequency is a classic triad—doctors trained in ovarian cancer recognize it immediately. One symptom alone is rarely enough for alarm; two or more persisting for weeks demand urgent evaluation.
Imagine 30 days from now: You’ve tracked subtle changes, spoken to your doctor confidently, had imaging done, and either ruled out cancer or caught it early—peace of mind restored, life ahead still full of possibility. The cost of inaction? Months or years of silent progression. The reward? Control, early intervention, and the best possible outcome.
Every day you wait to mention persistent symptoms gives cancer more time. Thousands of women have caught it early because they listened to their bodies—why not you?
Start today:
- Open your phone notes → start a 2-week symptom log.
- Write every day: bloating? fullness? urination changes? pelvic discomfort? fatigue? appetite shifts?
- If 2+ symptoms persist >2–3 weeks → call your doctor and say: “I’ve had persistent bloating, early satiety, and urinary frequency for weeks—I’d like to discuss ovarian cancer screening.”
- Request pelvic exam + transvaginal ultrasound ± CA-125.
- Don’t accept “it’s just IBS/menopause” without imaging if symptoms persist.
This article is for informational purposes only and does not replace professional medical advice. Ovarian cancer symptoms require accurate diagnosis—see your gynecologist or primary care provider promptly if you experience persistent changes. Early detection saves lives—never hesitate to advocate for yourself. Regular check-ups, family history discussion, and awareness are your best tools.
P.S. Ultimate insider tip: Bring your symptom diary + this list of 8 signs to your appointment—doctors respond faster to specific, documented patterns. Share your biggest “aha” moment or which sign surprised you most in the comments; your insight could help another woman act sooner. You deserve to be heard—and healthy.