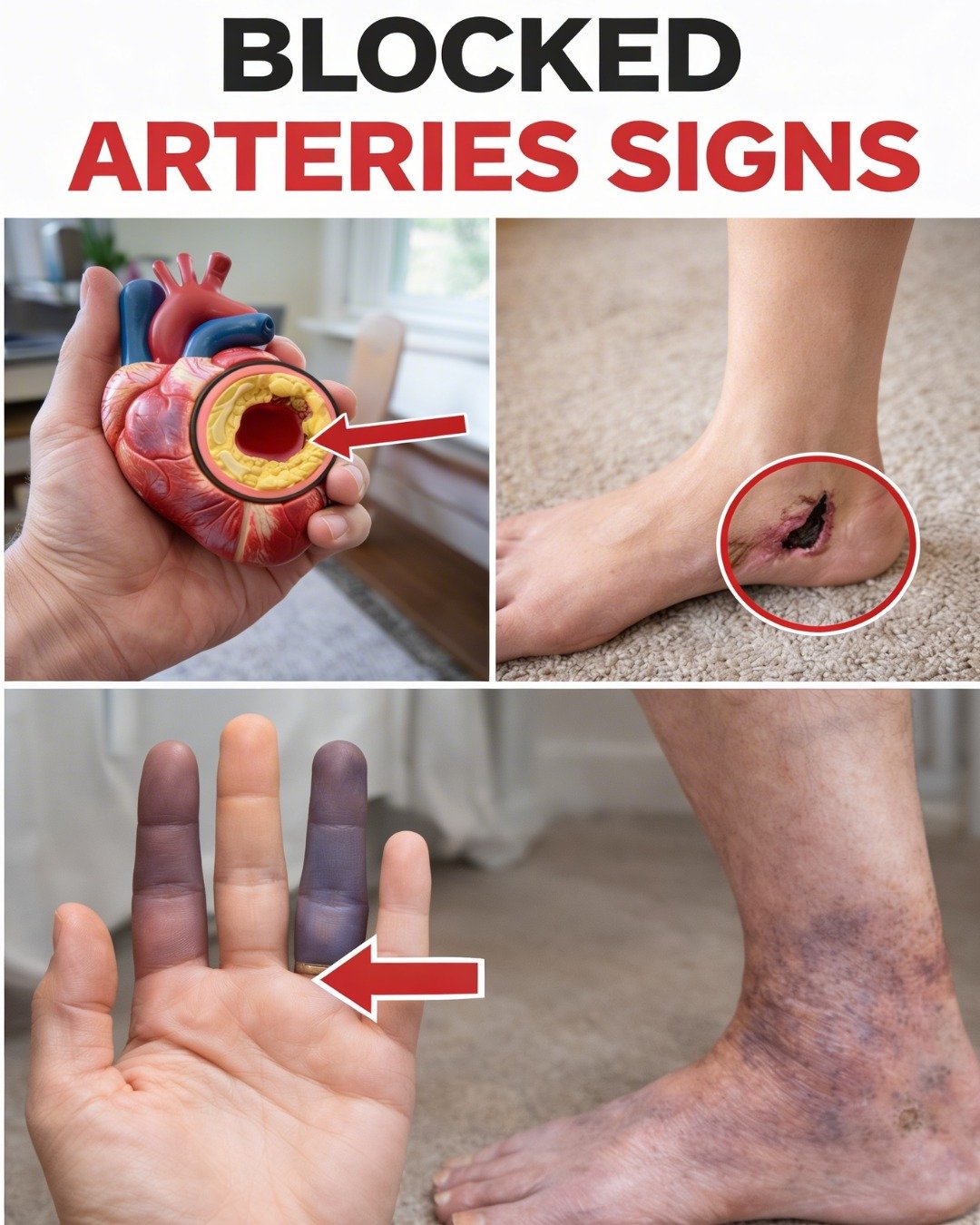
7 Early Warning Signs of Blocked Arteries in Legs and Feet You Should Know
Persistent leg discomfort, cold feet, or unusual skin changes can feel easy to ignore at first. Many people assume it is just aging, fatigue, or standing too long, but these subtle signals may point to reduced blood flow in the lower body. When circulation is limited, tissues do not receive enough oxygen, and over time that can affect mobility and overall heart health. The good news is that your body often sends clear clues before the problem becomes serious, and understanding these signs could make a meaningful difference, especially when you reach the final tip that many people overlook.

Understanding Blocked Arteries in the Legs and Feet
Blocked arteries in the legs are often linked to a condition known as peripheral artery disease. This happens when fatty deposits build up inside blood vessels, narrowing the space where blood flows.
According to the American Heart Association, reduced circulation in the lower limbs is common in adults over fifty, especially those with risk factors such as smoking, diabetes, high blood pressure, or high cholesterol. Studies suggest that many people have mild symptoms and do not realize what is happening.
Here is the key point. The earlier you recognize changes in your legs and feet, the sooner you can speak with a health professional and take steps to support your vascular health.
Why the Legs and Feet Show Symptoms First
The arteries in your legs are far from the heart. When blood vessels narrow, the lower limbs often feel the effects earlier than other areas.
Muscles in the calves and thighs need a steady supply of oxygen rich blood, especially when walking. If that supply drops, discomfort and visible changes can appear. And that is often where the first warning signs show up.
Let us break them down clearly.
1. Leg Pain While Walking That Improves With Rest
One of the most common early signs is pain, cramping, or heaviness in the calves, thighs, or buttocks when walking.
This pattern is important. The discomfort often appears after a certain distance and fades when you stop and rest. This happens because muscles demand more oxygen during movement, but narrowed arteries cannot deliver enough blood.
Researchers describe this as intermittent claudication. While the name sounds complex, the message is simple. Pain triggered by activity and relieved by rest should not be ignored.
But that is not all.

2. Cold Feet or Lower Legs
Do your feet feel noticeably colder than the rest of your body, even in warm weather
Reduced circulation can make one foot feel cooler than the other. You might notice that socks never seem warm enough or that your toes feel cold to the touch.
This happens because warm blood is not reaching the tissues efficiently. Over time, the skin may appear pale or slightly bluish.
If temperature differences are consistent rather than occasional, it may be worth paying attention.
3. Slow Healing Wounds or Sores
Small cuts, blisters, or sores on the feet should normally heal within a reasonable time. When blood flow is limited, healing slows down.
You may notice:
- A sore that stays open for weeks
- Cracks around the heels that do not improve
- Small wounds that look dry and stubborn
Healthy circulation supports tissue repair. Without enough oxygen and nutrients, the healing process struggles.
Here is why this matters. Slow healing in the feet can increase the risk of complications, especially for people with diabetes.
4. Changes in Skin Color or Texture
Skin can reveal a lot about circulation.
Some people notice:
- Pale or shiny skin on the legs
- A bluish or purplish tint on the toes
- Thin skin that looks tight or fragile
Reduced blood supply can also lead to hair loss on the lower legs. The skin may feel smooth and appear different from the rest of the body.
Studies in vascular medicine show that visible skin changes are often linked with moderate to advanced narrowing of the arteries.
And yet many people overlook them because the changes happen gradually.
5. Weak or Absent Pulse in the Feet
Health professionals often check pulses in the ankles and feet to assess circulation.
If you gently press on the top of your foot or behind the ankle, you may feel a subtle rhythm. In some cases of blocked arteries, that pulse becomes faint or difficult to detect.
While this is not always easy to check at home, it is a useful clue during routine examinations.
This is why regular checkups matter, especially if you have risk factors.
6. Numbness or Tingling in the Toes
A pins and needles sensation in the feet can have many causes, including nerve related issues. However, poor circulation can also contribute.
When blood flow is limited, nerves may not receive enough oxygen. This can lead to:
- Tingling sensations
- Burning feelings
- Unusual sensitivity
If numbness occurs alongside other symptoms such as cold feet or leg pain during walking, it becomes more relevant.
The truth is, symptoms often appear together rather than alone.
7. Severe Leg Pain at Rest in Later Stages
In more advanced cases, discomfort may occur even while resting, especially at night.
Some people describe a burning or aching feeling in the feet that improves when they hang their legs off the bed. This position allows gravity to help blood flow downward.
This stage signals significantly reduced circulation and requires prompt medical attention.
But here is the part many people do not realize.
Even mild early symptoms can signal broader cardiovascular risk.
The Connection Between Leg Arteries and Heart Health
Blocked arteries in the legs are not just a local issue. They can be a sign of widespread atherosclerosis, which affects blood vessels throughout the body.
Research published in major cardiology journals indicates that people with peripheral artery disease have a higher likelihood of heart related events compared to those without it.
That means recognizing leg symptoms early is not just about comfort. It is about understanding overall vascular health.
Here is a quick comparison to clarify:
| Symptom Pattern | What It May Suggest |
|---|---|
| Pain only after walking | Early reduced circulation |
| Cold and color changes | Ongoing blood flow limitation |
| Pain at rest | More advanced narrowing |
| Slow wound healing | Reduced oxygen delivery to tissues |
This table does not replace medical advice, but it helps you see patterns clearly.
Who Is at Higher Risk
Certain factors increase the likelihood of blocked arteries in the legs:
- Smoking
- Diabetes
- High blood pressure
- High cholesterol
- Family history of cardiovascular disease
- Age over fifty
If you fall into one or more of these categories, paying attention to subtle leg symptoms becomes even more important.
But do not panic.
Awareness is empowering.
Practical Steps You Can Take Today
You cannot change your genetics, but you can support your circulation with daily habits.
Here is a simple step by step approach:
Step 1 Pay Attention to Patterns
Notice when symptoms appear. Do they happen during walking. Do they improve with rest. Keeping a small journal for one week can reveal patterns.
Step 2 Support Healthy Movement
Engage in regular moderate physical activity such as brisk walking. Research shows that structured walking programs can improve circulation and endurance in people with mild symptoms.
Start slowly and increase gradually. Consistency matters more than intensity.
Step 3 Focus on Heart Friendly Nutrition
Choose foods that support vascular health:
- Leafy greens
- Whole grains
- Nuts and seeds
- Fatty fish rich in omega three
- Fruits with natural antioxidants
Limiting processed foods high in added sugars and unhealthy fats can also support overall circulation.
Step 4 Avoid Tobacco Exposure
Smoking is one of the strongest risk factors for artery narrowing. Reducing or quitting tobacco use significantly benefits blood vessel health over time.
Step 5 Schedule a Medical Evaluation
If you notice persistent symptoms, especially leg pain during walking or slow healing sores, speak with a qualified health professional. Simple non invasive tests can assess blood flow in the legs.
Early evaluation allows for personalized guidance tailored to your specific situation.
And here is the unexpected insight.
Many people focus only on pain, but subtle skin changes and cold feet often appear first. Recognizing these quiet signals can prompt earlier conversations and better long term awareness.
When to Seek Immediate Attention
While mild symptoms can be monitored, certain signs require urgent care:
- Sudden severe leg pain
- A foot that becomes pale and cold quickly
- Open sores with signs of infection
- Rapid worsening of symptoms
Prompt evaluation can help prevent complications.
Listening to your body is not overreacting. It is responsible self care.
Conclusion
Blocked arteries in the legs and feet often begin with subtle changes such as discomfort while walking, cold toes, or slow healing wounds. These signs may seem small, but together they can signal reduced circulation and broader cardiovascular risk. By recognizing early patterns, adopting heart supportive habits, and seeking timely medical advice, you can take proactive steps toward protecting your vascular health. The small details you notice today could shape your long term well being.
Frequently Asked Questions
1 Can blocked arteries in the legs cause symptoms without severe pain
Yes. Many people experience mild cramping, cold feet, or skin changes before significant pain appears. Early symptoms are often subtle.
2 Are cold feet always a sign of poor circulation
Not always. Temperature changes can result from environmental factors or nerve sensitivity. However, persistent coldness combined with other symptoms may suggest reduced blood flow.
3 How is blood flow in the legs usually evaluated
Health professionals may use a simple test called the ankle brachial index, which compares blood pressure in the ankle and arm. This helps assess circulation in a non invasive way.
Disclaimer
This article is for educational purposes only and is not a substitute for professional medical advice. Always consult a qualified healthcare provider regarding concerns about circulation or heart health.